Most unpleasant pains in the lumbar region and spine are associated with a disease such as osteochondrosis.It affects about 40% of men and women in their 30s and 40s and about 90% of older people.Therefore, the earlier the disease is diagnosed, the more thoroughly the patient is examined, the more likely it is to stop the development of osteochondrosis and maintain activity in old age.
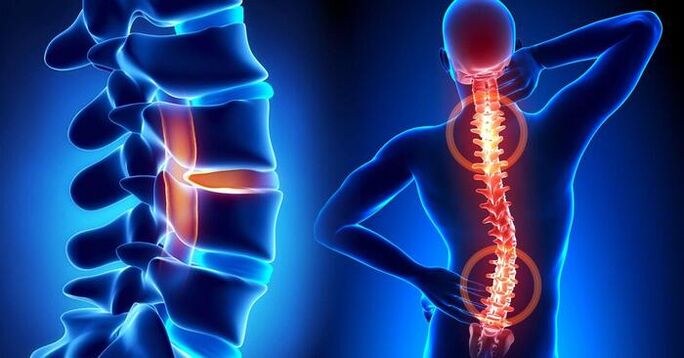
Definition of disease, cause of disease
So, what is osteochondrosis, where does it develop, what structures are affected, and what is the treatment method?The disease affects the tissues between the spine and vertebrae and is expressed by a violation of their shape, density, elasticity and sometimes even integrity.As a result, the distance between the vertebrae decreases, the spine gradually loses its stability, the nerves are compressed and the formation of hernias can develop, which is accompanied by back pain and discomfort during movement.
To briefly describe the essence of osteochondrosis, it is a gradual erosion of the tissues of the intervertebral discs (cartilage), causing instability of the spine.In the absence of treatment, degradation of ligaments and joints develops, osteophytes appear, posture is disturbed, movements are accompanied by pain.
Causes of spinal osteochondrosis:
- inactive lifestyle with lack of muscle load;
- spinal injuries;
- systematic heavy loads on the spine;
- heredity;
- overweight;
- hypothermia;
- hormonal and autoimmune diseases;
- toxic poisoning;
- congenital connective tissue deficiency;
- psychosomatic reasons (stress, depression, etc.).
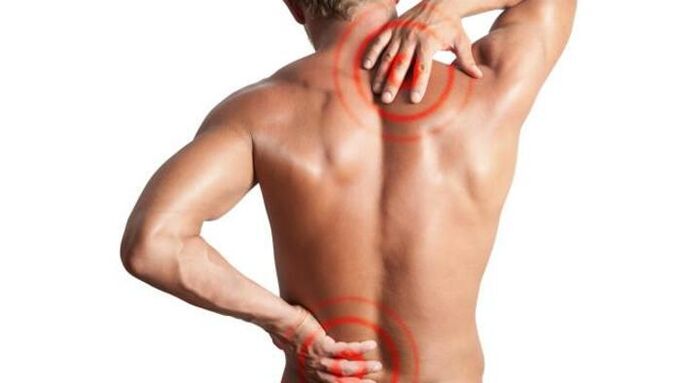
Symptoms of osteochondrosis
The disease is characterized by periods of remission and exacerbation with varying degrees of severity of symptoms.The main symptoms of spinal osteochondrosis are characteristic of the main types of the disease, the back, neck and chest area:
- localized pain in a certain region of the spine;
- pain syndrome associated with damage to nearby musculoskeletal tissues;
- myelopathy and radiculopathy caused by compression of the nerve endings of the spinal cord and blood vessels.
Depending on which part of the spine is affected by the disease, the list of symptoms of osteochondrosis may vary.Namely: patients report tingling in the muscles, numbness in the limbs, other sensory disturbances, weakness in the arms and legs, attacks of headache and heartache, painful back pain.
Pathogenesis of osteochondrosis
Before the elastic fibrous core of the intervertebral disc begins to lose its elasticity and deform, a number of processes that indicate osteochondrosis occur in the human body:
- spasms, dystonia, inflammation;
- decreased blood circulation;
- damage to nerve cell processes.
Then, the deformed annulus fibrosus develops cracks, disc protrusion, and herniation.Typically, such predisposing factors for spinal diseases develop during childhood or adolescence and are often the result of poor posture, scoliosis, sports injuries, infectious diseases or congenital vascular pathologies.

Stages of osteochondrosis
There are three stages of development of spinal osteochondrosis:
- first, the intervertebral disc begins to decrease in height, takes on a flat shape, loses moisture, elasticity, and may bulge;
- the second develops in the absence of treatment and is manifested by the disruption of the structure of the fibrous ring of the vertebral disc, the appearance of cracks and the development of instability of a certain area of the spine;
- characterized by the breaking of intervertebral cartilages, the development of hernia and the formation of bone processes of osteophytes.
The symptoms of the development of spinal osteochondrosis become more intense from the first stage to the third stage.
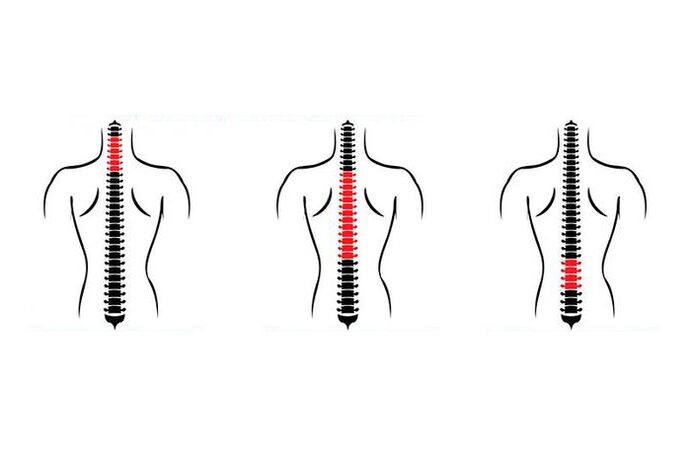
Classification of osteochondrosis
The classification of osteochondrosis is based on several signs, the main one of which is the localization zone.have:
- lumbar osteochondrosis;
- osteochondrosis of the cervical spine;
- osteochondrosis of the thoracic spine.
Osteochondrosis in the lumbar region is manifested by pain in the lumbar region, which increases when turning the body or lifting heavy objects.The pain may spread to the leg or both legs and is characterized as aching.A hernia is suspected in case of severe syndrome.With lumbar osteochondrosis, leg muscle spasms and skin peeling often occur.
With the development of spinal osteochondrosis in the cervical region, 1-7 vertebrae are affected.The disease is accompanied by a headache in the back of the head, pain in the neck, collarbones and shoulders.When turning the head, there may be a wheezing sound, numbness of the upper limbs, a feeling of swelling in the throat.
A patient with osteochondrosis of the spine in the thoracic region suffers from pain in the chest, shoulders, armpits and heart.There may be a feeling of difficulty breathing and the development of attacks of intercostal neuralgia.
Osteochondrosis is most common in the lumbar region, rarest in the thoracic spine.
Complications of osteochondrosis
If the patient thinks about treating osteochondrosis too late, when the symptoms of the disease are pronounced, the following complications may develop:
- intervertebral hernia;
- spinal cord stroke;
- spinal kyphosis;
- ledge;
- radiculitis;
- paralysis of the lower extremities.
In the absence of treatment, the patient begins to suffer from regular exacerbations of the condition, characterized by an increase in pain that interferes with movement and sharply worsens the general well-being.The most terrible complication of spinal osteochondrosis is disability.Therefore, high-quality and timely treatment of osteochondrosis is necessary to prevent such serious changes in the activity of the musculoskeletal system.
Diagnosis of osteochondrosis
A disease like osteochondrosis is primarily a pain in the spine.However, it is important to distinguish it from pain caused by problems unrelated to intervertebral disc degeneration.To do this, doctors carry out a step-by-step diagnosis, which includes:
- Don't date, involves a conversation between a specialist and a patient to determine the exact area of pain localization and the factors that cause the condition to worsen.It is important to know the occupation of the patient, when the problems related to the spine started, when there was an exacerbation, what pains occurred in the back and other areas, what treatment methods the patient used.
- Physiological examinationallows you to determine the proportions of the body, the quality of the performed movements and movements, the condition of the skin and the degree of pain sensitivity.The doctor uses palpation to determine the condition of the muscle tissue, the presence of compressions, swelling, etc.
- X-ray of the spine in two planesfor a visual assessment of its condition.It allows you to determine the displacement of the vertebrae, the presence of osteophytes and the deposition of salt.
If the collected information is not enough to determine the treatment or there is a suspicion of a serious pathology of the spine, CT and magnetic resonance imaging are prescribed to the patient, thanks to which it is possible to examine the spine, blood vessels, soft tissues, nerve processes in detail and create a complete picture of the condition of the affected osteodrosis of the spine.
Treatment of osteochondrosis
Like any disease, osteochondrosis requires determining the cause that led to its development.Reducing the severity of symptoms is not the main, but important stage of treatment, the result of which depends on a number of factors.In some cases it is a complete cure, in others it is prevention of complications and disability.
A group of measures are used in the treatment of spinal osteochondrosis:
- changing the patient's daily routine;
- prescribing drugs to reduce symptoms;
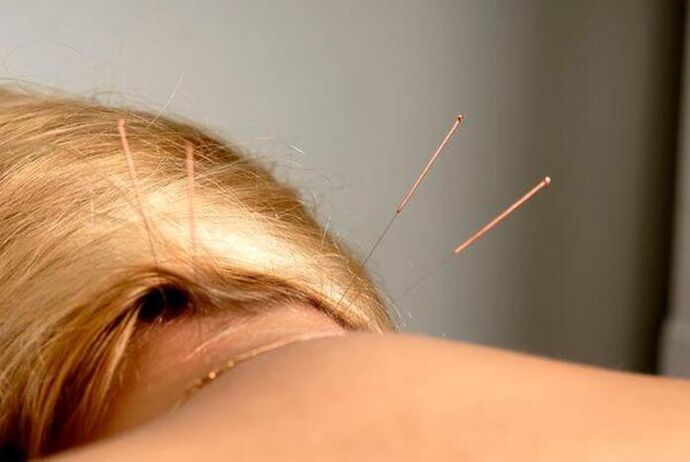
- physiotherapeutic procedures (massage, acupuncture, electrophoresis, exercise therapy, etc.).
Changing the daily routine in the treatment of spinal osteochondrosis involves reducing the intensity of physical activity, bed rest for severe pain, and avoiding sudden turns and bends.
Medicines for the treatment of spinal osteochondrosis
They can be divided into several groups:
- muscle relaxants to relieve pain, including tablets, injection anesthetics and anti-inflammatory injections for osteochondrosis.Homeopathic medicine normalizes the activity of the thyroid gland, improves lymphatic drainage, has an anti-inflammatory, detoxifying and immunomodulatory effect.
- non-steroidal anti-inflammatory drugs.When used in patients with osteoarthritis, there is a decrease in the course of inflammatory and destructive changes in the joints, improvement in the integrity, thickness and other properties of cartilage, and stimulation of bone tissue regeneration.
- anti-inflammatory ointments for topical applications and alternative transdermal patches.Such drugs have analgesic, antirheumatic, antipyretic and anti-inflammatory effects.The mechanism of action is to reduce the production of inflammatory mediators, reduce body temperature and pain.
- chondroprotectors;
- means for therapeutic analgesic blockades;
- B vitamins.
Supportive treatments
The most effective additional means that can be used to treat, relieve the general condition and improve the functioning of the spine and intervertebral discs are:
- acupuncture;
- magnetic therapy;
- professional massage and self-massage;
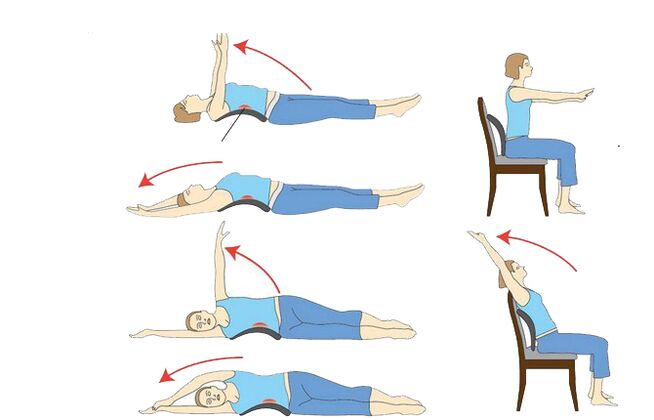
- physical education courses;
- manual therapy.
Prognosis, prevention
If the spinal disease does not progress and continues without serious complications, 1.5-2 months of competent treatment can significantly improve the condition and prevent the disease from becoming chronic.In difficult cases, doctors recommend surgical treatment.
Prevention of spinal osteochondrosis includes:
- maintaining the correct daily routine with changes in body position and moderate physical activity;
- regular visits to the pool;
- body weight control;
- wear comfortable shoes;
- balanced diet;
- sleeping on an orthopedic pillow and mattress;
- taking missing nutrients or preventive homeopathic medicines to boost immunity, improve general health and relieve dystonia.
Immediately after the appearance of any pain in the spine, it is necessary to undergo annual medical examinations and consult a doctor for treatment.
It doesn't matter which osteochondrosis we are talking about - back, neck or chest, taking care of your health should become a good habit, especially when it comes to the backbone of the entire musculoskeletal system - the spine.

























